High-Irradiance Photobiomodulation: Deep Tissue PBM Protocol Guide
SNIPPET: High-irradiance photobiomodulation (PBM) using Class IV lasers at wavelengths between 810–1215nm can deliver therapeutic fluence (6–10 J/cm²) to tissues 5cm deep, driving mitochondrial ATP synthesis, macrophage phenotype switching, and significant chronic pain reduction. A 2026 systematic review of 14 RCTs confirms PBM's analgesic efficacy, particularly for fibromyalgia and neuropathy, though protocol standardization remains the field's critical bottleneck.
THE PROTOHUMAN PERSPECTIVE#
Light is the oldest signal in biology. Before pharmaceuticals, before surgery, photons were already driving cellular respiration. And now we're finally learning to dose them properly.
High-irradiance photobiomodulation isn't new. What's new is the clinical precision — multi-wavelength diode arrays that differentiate between water absorption peaks and fat absorption windows, delivering energy not to the skin surface but to the deep tendons, joint capsules, and neural structures where pathology actually lives. For anyone serious about performance optimization, this shifts PBM from the "nice red light panel in the bathroom" category into something with genuine therapeutic architecture.
The data emerging in 2025–2026 matters because it addresses the single biggest failure in the PBM space: parameter chaos. Wavelength matters. Irradiance matters. Time matters. Tissue type matters. Most consumer devices get at least one of these catastrophically wrong. The research reviewed here starts to draw real lines around what works, at what dose, and for whom — and that's the only conversation worth having.
THE SCIENCE#
Photon Attenuation and the Depth Problem#
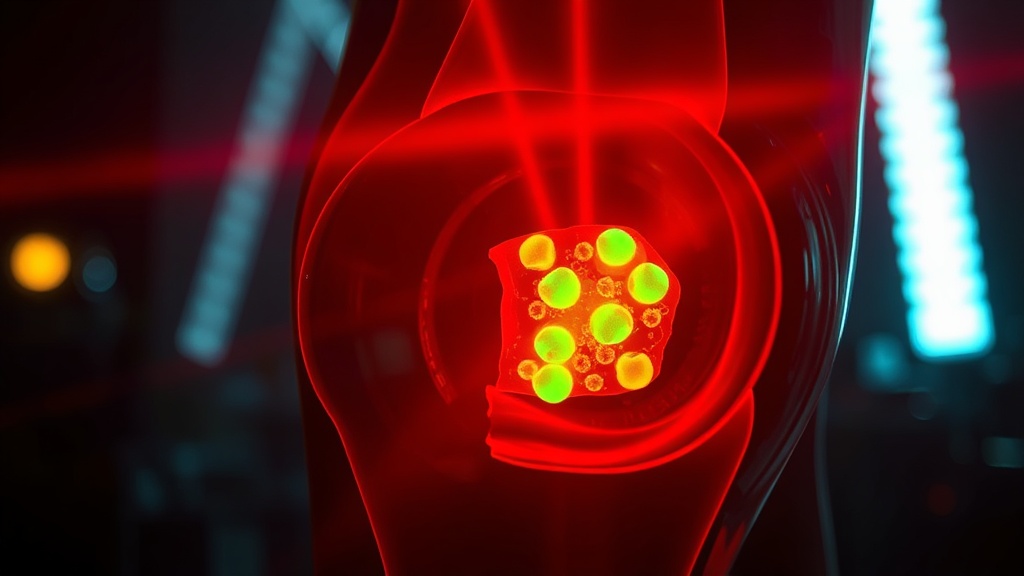
Photobiomodulation is the application of red or near-infrared (NIR) light to biological tissue to trigger photochemical responses — primarily through cytochrome c oxidase (Complex IV) in the mitochondrial electron transport chain. The core mechanism is well-established: photon absorption by CCO dissociates inhibitory nitric oxide, restoring oxygen binding and upregulating ATP synthesis[4][5].
But here's where most PBM discussions fall apart. They treat it as a surface phenomenon. The actual clinical challenge is photon delivery at depth.
Biological tissue is a scattering medium. The fluence at any given depth follows an exponential decay governed by the effective attenuation coefficient (μ_eff). The equation is straightforward: Φ(z) ≈ Φ₀ · 3 · e^(−μ_eff · z). What this means in practice is that a low-power LED panel delivering 50 mW/cm² at the skin surface has essentially zero therapeutic photons reaching a hip joint capsule at 5cm depth[1].
Class IV laser systems — operating at 10–60W output — exist to solve this specific physics problem. They maintain sufficient photon density so that the "tail" of the energy curve still falls within the therapeutic window of 6–10 J/cm² at the target tissue. Without that initial wattage, you're irradiating skin and subcutaneous fat. Period.
The Biphasic Dose Response: Why More Isn't Better#
The Arndt-Schulz law governs PBM dosing and it's non-negotiable. Too little energy: no biological response. Too much: inhibition and potential tissue damage. This biphasic curve is the reason I get frustrated with both the "more power = better" crowd and the "any red light works" minimalists[1].
The therapeutic window is narrow, and it shifts based on tissue type, pigmentation, adiposity, and target depth. A protocol that works on a lean 70kg male athlete's knee may be entirely wrong for a 95kg post-surgical patient with significant subcutaneous fat over the same joint.
Multi-Wavelength Clinical Synergies#
The data from multi-wavelength platforms reveals something the single-wavelength crowd misses entirely[1]:
- 1215nm ("Fat Peak"): Minimal absorption by melanin and hemoglobin. Maximum penetration through adipose tissue. This is your deep biostimulation wavelength — reaching bone, deep tendons, and structures buried under fat layers that 810nm or 980nm cannot efficiently access.
- 1470nm ("Water Peak"): High absorption coefficient in water. Useful for surgical precision and superficial tissue ablation, but not for deep penetration protocols.
- 910–980nm (Oxygenation range): Absorbed by cytochrome c oxidase. The classic PBM wavelength range for mitochondrial activation, modulating the inflammatory cascade and driving the M1-to-M2 macrophage phenotype switch.
The catch, though. Most studies still use single-wavelength protocols, which makes it nearly impossible to validate the claimed synergies of multi-wavelength systems with rigorous comparative data. I'd want to see head-to-head RCTs — same pathology, same patient population, single vs. multi-wavelength — before calling this settled.

Chronic Pain: What 14 RCTs Actually Show#
The Cabral Oliveira et al. (2026) systematic review is the most current synthesis — 14 randomized clinical trials covering fibromyalgia, peripheral neuropathies, orofacial pain, and musculoskeletal conditions[2].
The headline: most trials demonstrated significant pain reduction with PBM, particularly in fibromyalgia and neuropathy. Some studies also reported functional gains and improved quality of life. Adverse event incidence was low.
But let me push back on the enthusiasm. "Most trials" is not "all trials." The review explicitly flags that heterogeneity of technical parameters compromises standardization. Translation: different studies used different wavelengths, different power densities, different treatment durations, different spot sizes — and we're comparing their results as if they tested the same intervention. They didn't.
The WALT Position Paper from Hanna, Chow, Hamblin et al. (2026) narrows the focus to orofacial neuropathic pain and provides more specific dosing guidance, but even this expert consensus acknowledges the parameter standardization problem[3].
Neural Modulation and the CNS Frontier#
Zhang et al. (2025) analyzed 150 PubMed-indexed studies on PBM's effects on the central nervous system, including 46 clinical trials[4]. The mechanisms are consistent with peripheral applications: enhanced ATP synthesis, modulated nitric oxide signaling, suppressed oxidative stress, and anti-inflammatory effects.
What's genuinely interesting — and surprised me — is the preliminary data on treatment-resistant depression. An open-label study by researchers publishing in Lasers in Medical Science used a high-power 850nm device (5000 mW output, 127 mW/cm² irradiance) applied transcranially for just 2 minutes per session[6]. Seven patients with treatment-resistant depression showed median HAM-D scores dropping from 23 to 9 after four weeks.
I need to be honest about the limitations here. n=7. Open-label. No control group. No blinding. The p-values didn't even reach conventional significance (P = 0.09 for mean scores). This is hypothesis-generating at best. But a median drop from 23 to 9 on the Hamilton scale — that's a move from moderate-severe depression to near-remission. If that replicates in a proper RCT, the implications for neuropsychiatry are substantial.
HAM-D Score Change After Transcranial PBM (n=7)
COMPARISON TABLE#
| Method | Mechanism | Evidence Level | Cost | Accessibility |
|---|---|---|---|---|
| High-Irradiance Class IV PBM (multi-wavelength) | Cytochrome c oxidase activation, macrophage M1→M2 switching, deep tissue ATP synthesis | Moderate (systematic reviews + RCTs, parameter heterogeneity) | $15,000–$80,000 (clinical systems) | Clinical settings only |
| Low-Level Laser Therapy (LLLT, Class IIIb) | Same CCO mechanism, limited to superficial tissue (1–2cm) | Moderate-High (larger evidence base, but for superficial targets) | $2,000–$10,000 | Clinical + some home devices |
| Consumer LED Panels (red/NIR) | CCO activation at skin/subcutaneous level only | Low-Moderate (mostly skin/cosmetic evidence) | $200–$2,000 | Home use, widely available |
| Transcranial PBM (tPBM) | Cortical CCO activation, NO modulation, neuroinflammation reduction | Low (small pilot studies, no large RCTs) | $500–$5,000 | Emerging home/clinical devices |
| NSAIDs/Pharmacological | COX inhibition, systemic anti-inflammatory | High (extensive RCT evidence) | $5–$50/month | OTC and prescription |
THE PROTOCOL#
For individuals considering high-irradiance PBM for deep tissue pain or recovery optimization — based on current evidence and clinical parameters reported across the reviewed studies.
1. Confirm the target depth and select wavelength accordingly. Superficial targets (skin, shallow muscle, < 2cm): 630–660nm red or 810nm NIR is adequate at lower power. Deep targets (joints, deep tendons, bone, > 3cm): you need 910–1215nm NIR from a Class IV source delivering ≥ 10W output power.
2. Establish your target fluence at tissue depth, not at the skin surface. The therapeutic window for deep tissue PBM appears to be 6–10 J/cm² at the target. Because of exponential attenuation, you may need surface fluences of 30–60 J/cm² to achieve this. Calculate based on your device's known attenuation data for the specific wavelength and tissue type.
3. Use continuous wave for deep tissue; consider pulsed for neural applications. The depression study used 10 Hz pulsed delivery at 850nm for transcranial applications[6]. For musculoskeletal targets, continuous wave at 910–980nm appears to be the more common clinical protocol in the reviewed RCTs[2].
4. Treatment duration: match energy delivery to target area. Most clinical protocols in the Cabral Oliveira review used sessions ranging from 30 seconds to 10 minutes per point, depending on power output. Higher wattage = shorter treatment time for the same energy dose. A 30W system delivering to a knee joint may need only 60–90 seconds per treatment point.
5. Session frequency: 2–3 times per week for chronic conditions. Based on the protocols reported in the systematic review, most successful trials used 2–3 sessions per week over 4–8 weeks[2]. Daily treatment was used in the transcranial depression protocol (8 sessions over the study period)[6].
6. Monitor and adjust based on response. The biphasic dose-response means more is not better. If symptoms worsen or plateau, reduce fluence before increasing it. Track pain scores (VAS/NRS) and functional outcomes weekly.
7. Safety: eye protection is non-negotiable with Class IV systems. Both operator and patient require appropriate optical density (OD) rated eyewear for the specific wavelength in use. Avoid direct irradiation over the thyroid, testes, or active malignancies. Consult a trained practitioner — this is not a consumer LED panel protocol.
Related Video
What is high-irradiance photobiomodulation and how does it differ from regular red light therapy?#
High-irradiance PBM uses Class IV laser systems delivering 10–60W of output power at specific near-infrared wavelengths. Unlike consumer LED panels that only penetrate 1–2cm, these systems push sufficient photon density to reach tissues at 5cm or deeper — joints, deep tendons, nerve structures. The mechanism is the same (cytochrome c oxidase activation), but the clinical reach is entirely different.
Why does wavelength selection matter so much in PBM?#
Different wavelengths are absorbed differently by water, hemoglobin, melanin, and fat. A 1215nm laser passes through adipose tissue with minimal absorption, reaching deep structures. A 1470nm laser is heavily absorbed by water, making it useful for surgical precision but poor for depth penetration[1]. Getting the wavelength wrong means your photons never reach the target — you're heating surface tissue for nothing.
How strong is the evidence for PBM in chronic pain management?#
A 2026 systematic review of 14 RCTs found that most trials showed significant pain reduction, especially in fibromyalgia and neuropathy[2]. The safety profile is strong with low adverse events. However, the heterogeneity of protocols across studies remains a real limitation — we don't yet have a single "gold standard" dosing protocol for any specific condition.
Can photobiomodulation help with depression?#
Preliminary data suggests it may. One small open-label study (n=7) using high-power 850nm transcranial PBM reduced median HAM-D depression scores from 23 to 9 over four weeks[6]. But this was uncontrolled, unblinded, and didn't reach statistical significance. It's an intriguing signal that needs proper RCT validation before anyone should consider it a treatment option.
Who should avoid high-irradiance PBM treatment?#
Individuals with active malignancies in the treatment area, pregnant women (over the uterus), those with photosensitivity disorders, and anyone on photosensitizing medications should avoid or exercise extreme caution. Class IV laser treatment requires trained clinical supervision — the power densities involved can cause retinal damage and thermal burns if misapplied.
VERDICT#
Score: 6.5/10
The physics is sound. The mechanism is well-characterized. The clinical signals are real — particularly for chronic pain conditions where conventional pharmacology fails or carries unacceptable side effects. I'm genuinely encouraged by the multi-wavelength approach and the emerging neuropsychiatric applications.
But I can't score this higher when the field's own systematic reviews keep flagging the same problem: parameter chaos. Fourteen RCTs using fourteen different protocols isn't an evidence base — it's fourteen separate anecdotes wearing lab coats. Until we get standardized dosing guidelines from properly powered multicenter trials, high-irradiance PBM remains a therapy with legitimate potential that's being undermined by its own lack of methodological discipline. The consumer market confusion only compounds this. I've used PBM personally and believe in the mechanism. I just don't believe we've earned the right to prescribe with confidence yet.
References
- 2.Cabral Oliveira AB, Nogueira Santos G, Ferreira LMA, Mendes JJB, Costa GV, Silva IR, Pereira GS, Silva ML. Photobiomodulation in chronic pain: a systematic review of randomized clinical trials. Frontiers in Integrative Neuroscience (2026). ↩
- 3.Hanna R, Chow R, Dalvi S, Arany PR, Bensadoun RJ, Santos-Silva AR, Tunér J, Carroll JD, Hamblin MR, Anders J, Rochkind S, Heiskanen V, Raber-Durlacher JE, Laakso EL. Photobiomodulation Therapy in the Management of Orofacial Neuropathic Pain—WALT Position Paper 2026. Journal of Clinical Medicine (2026). ↩
- 4.Zhang Z, Xue X, Liu P, Zhang C, Li J, Liu Y, Jiang Y, Lv S, Wang L, Zhou H, Shen W, Yang S, Wang F. The role of photobiomodulation in modulating neural activity and brain function: A systematic bibliometric analysis. Photodiagnosis and Photodynamic Therapy (2025). ↩
- 5.Martins DO, Rocha IRC, Watkins LR, Chacur M. Photobiomodulation therapy in neuropathic pain: mechanisms, evidence, and future directions. Frontiers in Photonics (2025). ↩
- 6.Author(s) not listed. A high-power near-infrared photobiomodulation device: design, fabrication, and primary impact on treatment-resistant depression. Lasers in Medical Science (2025). ↩
Sova Reld
Sova writes with focused intensity and low tolerance for vague claims. She came to photobiomodulation through personal experimentation and is irritated by both true believers and reflexive skeptics. Her writing has edge: 'The wellness market has done more damage to this field than the skeptics ever could.' She's extremely precise about parameters — wavelength, irradiance, duration — and will tell you when a study used inadequate dosing without apology.
View all articles →